On Rural Women’s Healthcare Access, Robotics in Medicine
During a recent White House press briefing, Dr. Mehmet Oz promoted an automated fix for a growing women’s health concern.
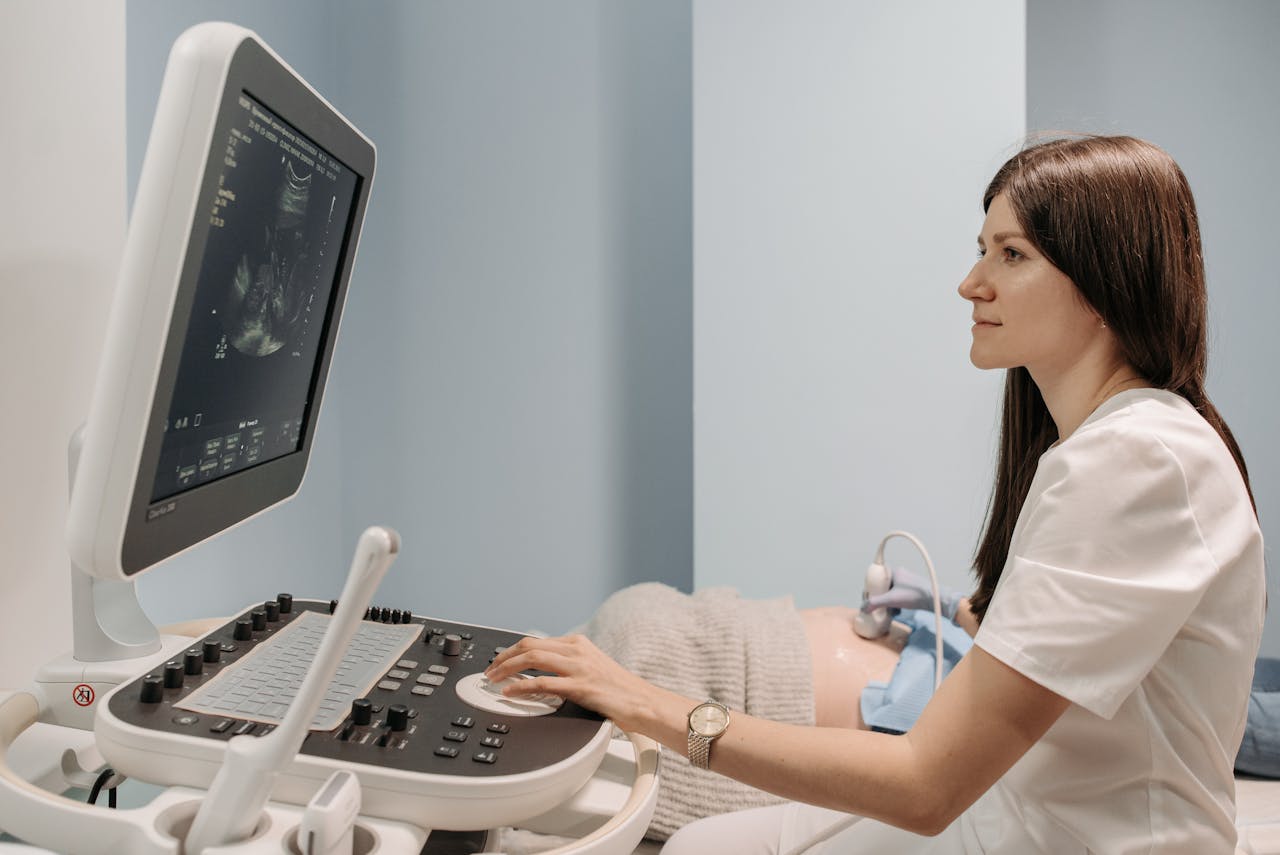
The television-personality-turned-administrator for Medicare and Medicaid told reporters, while seated with President Donald Trump and Health Secretary Robert F. Kennedy Jr., that “Alabama has no OBGYNs in many of their counties, so they’re doing something pretty cool: They’re actually having robots do ultrasounds on these pregnant moms.”
Oz was referring to a real proposal to use federal funds in Alabama to create “telerobotic ultrasound systems.” But several lawmakers, including Vermont Sen. Bernie Sanders, took issue with Oz’s framing of the subject.
“No, Dr. Oz. It is not ‘cool’ that we don’t have OBGYNs in many rural counties in America. It is an international embarrassment,” Sanders said in a statement. “In the richest country on Earth, we need more doctors, nurses, dentists and mental health counselors – not more robots.”
A Growing Problem, For Women Especially
Rural areas of the country – which are defined by a region’s remoteness and smaller population size – have been healthcare deserts for decades. “In rural areas, you have to travel further distances to access care, wait longer to be seen, and fewer services” are on offer, says Eileen Barrett, president of the American Medical Women’s Association. Making matters worse is the fact that residents of rural counties are disproportionately poor, and are more frequently unable to afford healthcare.
Under the second Trump administration, the situation has gotten worse. As a result of policies and funding cuts enacted in 2025, clinics are closing – at least 36 facilities shut down last year throughout the nation, as well as about 50 Planned Parenthood locations. Hundreds more are at risk. This means “delayed [or] foregone care, worse health outcomes and financial hardship for families,” the American Medical Association said in a statement on how Trump’s 2025 policies are impacting patients.
Accessing practitioners has long been a problem in and of itself for rural residents, according to Kris Pakaart, who works in behavioral health at Gallup Community Health, a healthcare facility in northwestern New Mexico. Though her offices have the capacity to help more people, “we cannot get patients in, as many rural areas don’t have a public-transport infrastructure” like buses or trains that would allow them to even get to appointments, she says.
Exacerbating that problem is the impending loss of Covid-lockdown-era telehealth protections – permissions for the use of audio-only calls, flexibilities around the respective locations of patients and practitioners and more, all of which are set to expire later this month.
But like robots, even telehealth visits aren’t an ideal tech-based solution, as WiFi access is unreliable in rural parts of the nation – about 22.3% of those living in these parts of the country having no internet access at all. Also, many are left trying to shoehorn remote visits in around their home- and childcare responsibilities, women in particular. “I can hear how distracted [patients] are. It’s difficult, doing five things at once,” Pakaart says.
Gynecological, obstetric, labor and delivery services come with additional, unique hindrances, says Marcie Richmond, a family physician and the director of training programs at Gallup Community Health. Such offerings are even more difficult and costly to offer – in all parts of the nation – largely for liability reasons, but also because of the sheer number of on-call nurses and surgeons needed for parents and children.
Compounding that portion of the problem is the repeal of Roe v. Wade, which has caused a brain drain in states with the most prohibitive abortion laws – many of them home to the country’s most rural areas – because fewer medical professionals are applying to residencies and jobs in these regions.
The combined result: “When care is harder to access, the outcomes are worse” for patients, Barrett says – potentially deadly, even.
A Call for Humane – and Human – Solutions
When it comes to fixing this crisis, “I always support innovation that is grounded in patient safety and that honors patient preferences,” Barrett offers, in regards to the robotic solution Oz promoted, adding that “there is guidance from the Society for Maternal-Fetal Medicine on the use of tele-ultrasound that acknowledges this is very promising.”
But, she continued, “we should also be talking about how to leverage collaborations with inter-professional colleagues” like midwives, as well as “a community pilot [program] that offers women-friendly workplaces such as employer-funded childcare, infertility treatment coverage, expansive parental leave, and after-school activities” to incentivize practitioners to work in these parts of the country.
A 2025 study on rural healthcare access, published in the American Journal of Medicine, also pointed to mobile clinics and travel subsidies for patients, to address some of the transportation- and cost-related barriers to access.
A holistic and human approach would be best, experts agree. Richmond adds that, in many cases – especially when it comes to gynecology and obstetrics – a robot would simply come with too many risks. Everything from physical examinations and placements of contraceptive devices, to performing surgical abortions, hysterectomies and biopsies, all require “on-site, hands-on, skilled practitioners.”
And, she adds, robotics are simply too impersonal. “I really value being able to be physically at my patients’ sides as we travel their health journeys together,” she said. “Reproductive healthcare is often intense. Being able to hold a hand, offer a tissue, or just hold physical presence for my patients is an essential part of providing healthcare to me.” ◼️
link






